Acute appendicitis is the sudden, severe inflammation of the appendix, typically causing pain that starts around the navel and moves to the right lower abdomen. It is a surgical emergency often caused by blockage, requiring immediate diagnosis via imaging (CT/sonography) and treatment (usually surgery) to prevent rupture, which can lead to life-threatening infections.
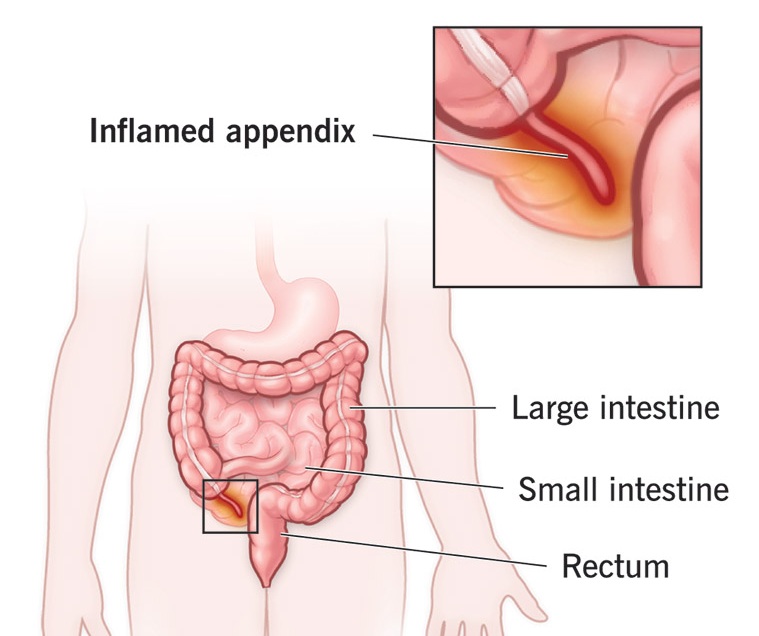
Key Symptoms of Acute Appendicitis
Abdominal pain: Usually begins as dull pain near the belly button, moving to the right lower abdomen, becoming sharp and severe.
Worsening pain: The pain increases with walking, coughing, or sudden movements.
Digestive distress: Nausea, vomiting, loss of appetite, and sometimes diarrhea or constipation.
Fever: Often a low-grade fever that may increase if the infection worsens.
Abdominal swelling: The belly may feel bloated or tender.
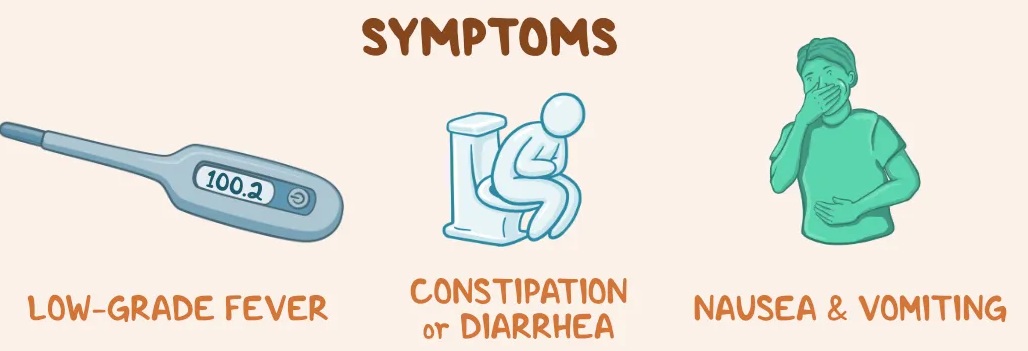
The early signs of appendicitis
In the typical presentation, abdominal pain begins in the middle of your abdomen, around your belly button. It may hover or may come and go for several hours. Eventually, the pain intensifies, and nausea and vomiting develop. Several hours later, the nausea passes, and the pain shifts to your lower right abdomen, where your appendix is. The pain becomes more focused and continues to worsen.
Other possible symptoms of appendicitis
Fever
Up to 40% of people develop a fever. This means your immune system is kicking into a higher gear. It may also mean inflammation is increasing or it may mean infection is spreading.
Malaise
You may just notice that you feel generally unwell. You may lack energy or motivation and feel like staying in bed, the way you do when you’re sick.
Swollen belly
Your abdomen may look distended or feel bloated. This is usually an advanced symptom and may indicate your appendix has ruptured.
Urinary symptoms. You may feel like you have to pee more often or more urgently. This can happen if appendicitis irritates nerves connected to your bladder.
Bowel paralysis
When your body redirects blood flow from your bowels to your appendix, your bowels can temporarily stop moving. Some people develop constipation and feel that they can’t pass gas. You may have the sense that a bowel movement would relieve your symptoms.
Diarrhea
Some people may have overactive bowels and more frequent poops. This may be because inflammation from your appendix is irritating the end portion of your colon beside it.
Causes and Risk Factors
Blockage
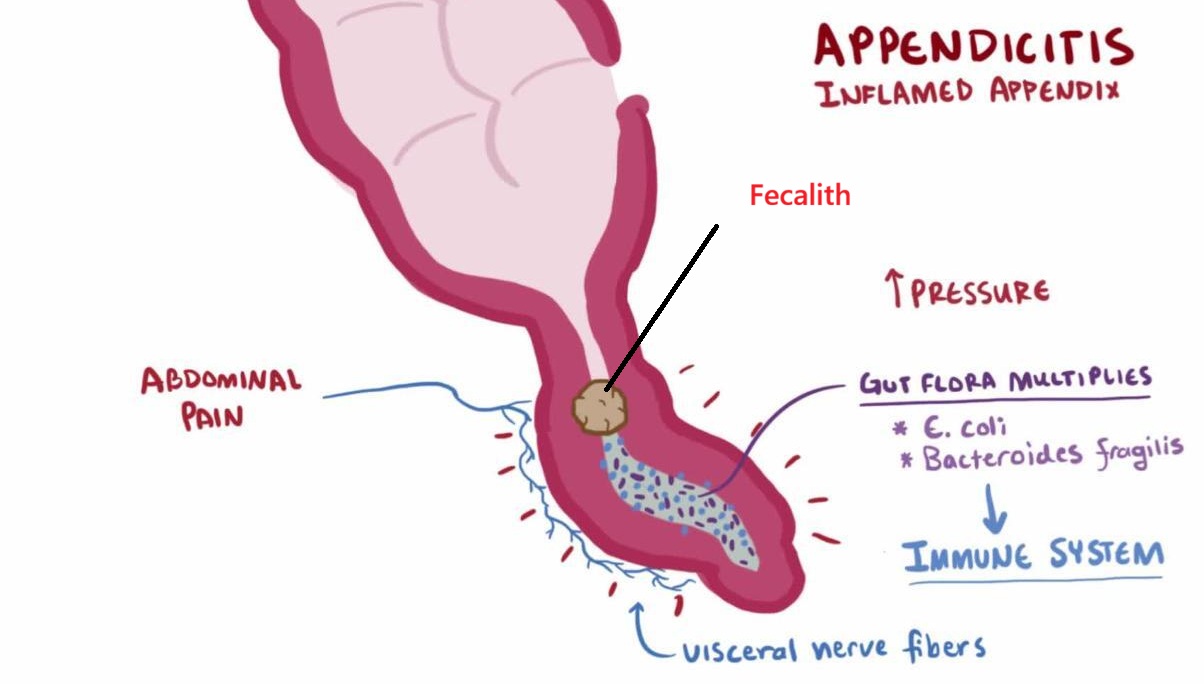
A blockage in the lining of the appendix (caused by fecalith, lymphoid hyperplasia, or rarely tumors) is the most common cause, causing bacteria to multiply and the appendix to fill with pus.
Age/Sex: It most commonly happens between the ages of 10 and 30, with males having a slightly higher risk than females.
Burst appendix
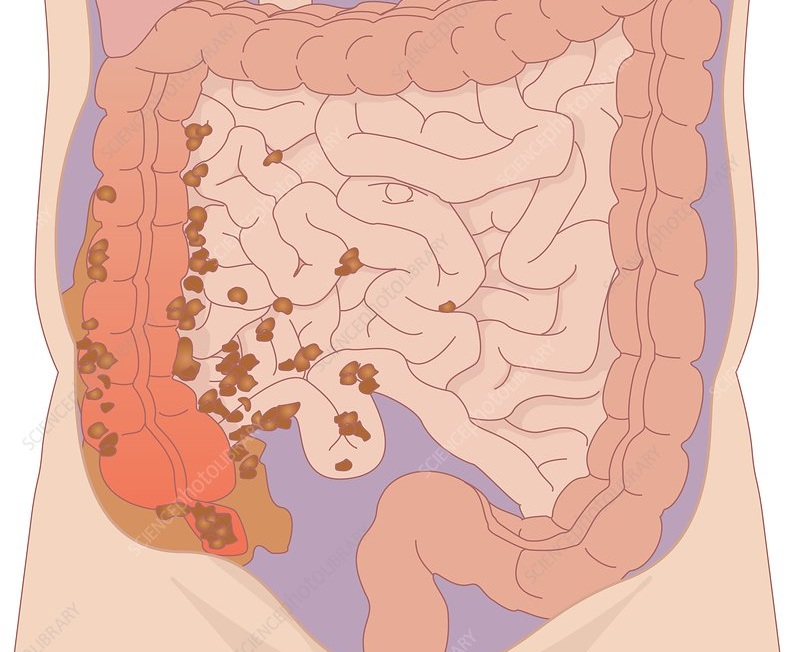
A burst appendix is a medical emergency. It spreads bacteria from inside your bowels throughout your abdominal cavity. This infection (peritonitis) can then spread to your bloodstream, which can lead to life-threatening complications (sepsis). Because of this risk, the standard treatment for appendicitis is to remove your appendix (appendectomy). Your appendix isn’t an essential organ, and you won’t miss it.
The size and location of your appendix make it easy for it to become clogged and infected. Your large intestine is home to many bacteria, and if too many become trapped in your appendix, they overgrow and cause an infection. Sometimes, appendicitis begins with an infection, and sometimes, the infection is secondary. Swelling in your appendix can reduce or close the opening and trap more bacteria inside.
Common causes of inflammation, swelling, obstruction and infection in your appendix
Hardened poop (appendix stones)
Hard, calcified fecal deposits known as fecaliths, appendicoliths or appendix stones can get stuck in the opening to your appendix. They carry bacteria and can also trap bacteria that was already there inside your appendix.
Lymphoid hyperplasia
Your lymphatic system, which is part of your immune system, helps fight infections by producing and releasing white blood cells into your tissues. This can cause the lymphoid tissue in your appendix to swell, even when the original infection is elsewhere in your body. The swollen tissue in your appendix can obstruct it and lead to infection inside.
Colitis
Inflammation in your colon from an infection or inflammatory bowel disease can affect your appendix. The infection may spread, or the inflammation itself may irritate it.
Other factors that could block the opening to your appendix
Tumors.
Parasites.
Cystic fibrosis.
Acute appendicitis and chronic appendicitis
Appendicitis is almost always an acute condition, which means it begins suddenly and worsens quickly. Most of what we know about appendicitis refers to acute appendicitis, which is very common. Chronic appendicitis is a rare condition that we don’t know as much about. It appears to occur when something irritates your appendix in an on-and-off sort of way over a long period, but it never gets worse.
Chronic appendicitis may go unrecognized because the symptoms don’t escalate the way they do in acute appendicitis. But any type of appendicitis is serious. Chronic abdominal pain and don’t know what causes it, it’s important to consult a physician. Chronic appendicitis may worsen or become acute at any time.
Diagnosis of acute appendicitis
Physical examinations
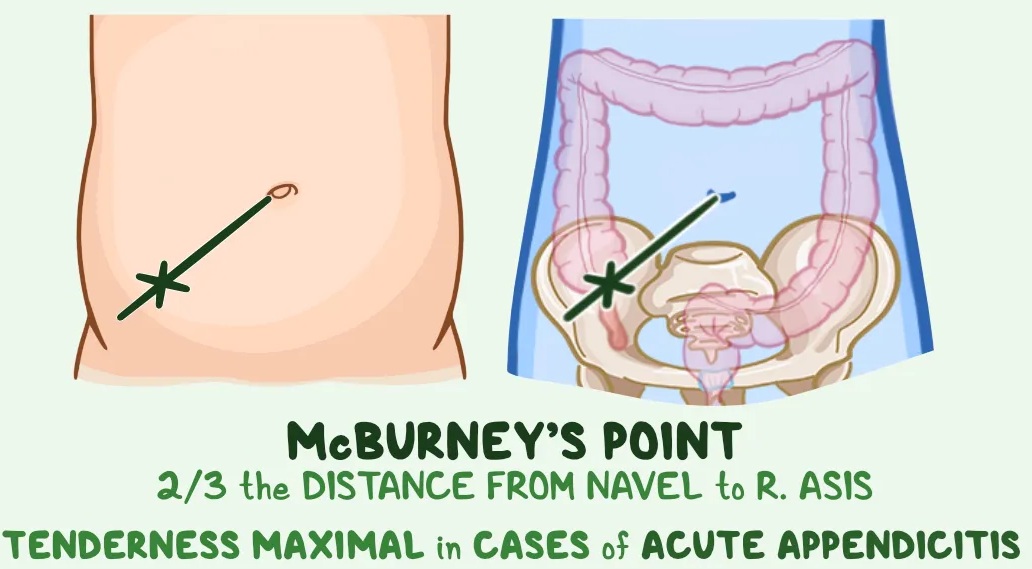
McBurney’s sign
McBurney’s point is the most typical location of the appendix, and tenderness there is the first thing healthcare providers check for in a physical exam. They find it by drawing a line from your ASIS (a bony projection near your hip) to your belly button and measuring the distance. The point is about two inches along the line, or one-third of the distance.
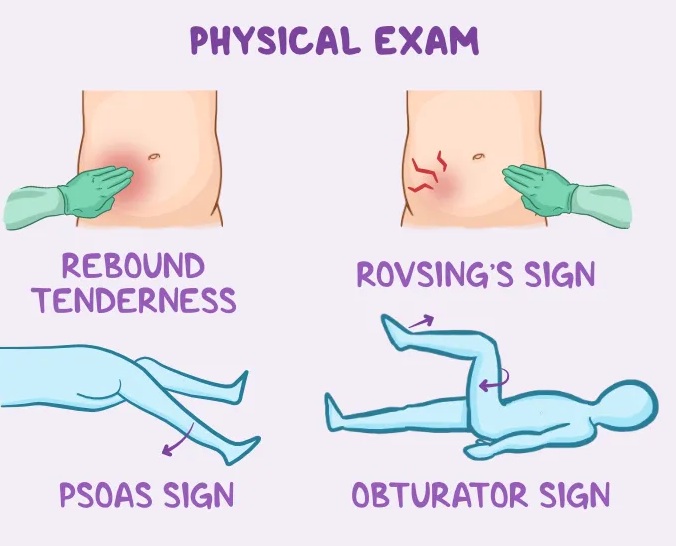
Blumberg’s sign
Pressure applied to the sore area feels worse when it’s released (also known as rebound tenderness).
Dunphy’s sign
Coughing makes the pain worse.
Rovsing’s sign
Pressure on your lower left side produces pain on your lower right side.
Psoas sign
If your appendix is behind your colon rather than in front, appendicitis might irritate your psoas muscle. You might find yourself flexing your right hip to shorten the muscle, which relieves pain. A healthcare provider might try extending your right hip or rotating it outward. If this hurts, it’s called the psoas sign. If rotating it inward hurts, it’s called the obturator sign.
Laboratory Investigations
Blood test and urine test
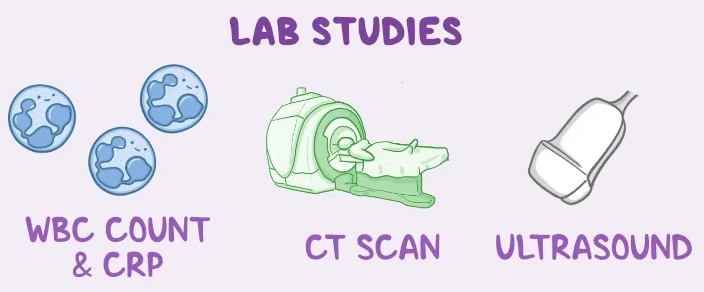
Imaging techniques
CT scans or abdominal sonography.
Other conditions might be confused with appendicitis
Symptoms of appendicitis can resemble many other conditions. This is especially true for females. Your lower abdomen lies close to your pelvic cavity, and conditions affecting your pelvic organs may feel very similar to appendicitis. These organs include your urinary system and female reproductive system. Other lower abdominal organs may also be involved.
Pelvic inflammatory disease.
Endometriosis.
Ovarian cyst.
Kidney stone.
Urinary tract infection.
Pancreatitis.
Inflammatory bowel disease.
Diverticulitis of the colon.
Gastroenteritis.
Intestinal obstruction.
The possible complications of appendicitis
Appendicitis can quickly lead to very serious complications, it as an emergency. Complications can progress in stages, though they don’t always happen in the same way.
Complications (stages)
Ischemia and necrosis
Severe swelling in your appendix cuts off the blood supply (ischemia,) which increases inflammation and eventually causes the tissues to start to decay (necrosis).
Gangrene/perforation
Once necrosis sets in, infection can spread. It may spread slowly through internal gangrene or quickly when your appendix tears or bursts (perforation).
Abscess/phlegmon
At first, the infection might not spread far beyond your appendix. It might form an abscess, a pocket of pus, on the outside of your appendix. The appendix can also develop a mass around itself called a phlegmon. These masses contain the infection, but they can burst.
Peritonitis and spreading infection
When infection spreads into your peritoneal cavity (peritonitis), it can spread to other organs and even to your bloodstream (septicemia). Infection in your bloodstream can lead to sepsis and septic shock, which can be fatal.
Treatment for Acute appendicitis
The standard, most effective treatment is a laparoscopic appendectomy, which is the surgical removal of the appendix.
Appendicitis is considered an emergency, so it’s treated in the emergency room. The standard treatment includes both medication and surgery, though in a small number of cases, medication might be enough.
Medication
Almost everyone will need antibiotics for appendicitis. Even if you didn’t have an infection to start with, appendicitis usually leads to one. Antibiotics are also a standard preventive treatment before surgery.
If you have a very early and mild case of appendicitis, your healthcare provider might take a wait-and-watch approach to see if your condition improves with antibiotics alone. You might prefer this approach if you have risk factors that make surgery less safe for you. However, healthcare providers rarely recommend it because appendicitis often returns when you don’t have your appendix removed.
You may also need medication for pain relief. You can have this through your IV. If you’re having surgery, you’ll have general anesthesia, so you won’t be conscious (awake) during the procedure.
Surgery
Diagnosed with appendicitis, time is of the essence. Your appendix can rupture within 36 hours of your first symptoms. Surgeons will usually schedule your appendectomy within 24 hours of your diagnosis. Appendectomy is one of the most common surgical procedures performed worldwide. Surgeons can often perform it using minimally invasive methods, such as laparoscopic surgery.
Treat any complications you have during your surgery. Complications may require open abdominal surgery to manage. After surgery, they’ll rinse your abdomen with a sterile solution.
There aren’t any side effects of having your appendix removed. Not sure appendix has any function. If it does, it’s a small one. It may help make antibodies during childhood.
Prognosis of Acute appendicitis
Prognosis is generally excellent if treated promptly, but delay can lead to a ruptured appendix and severe infection (peritonitis).
With early recognition and treatment, the outlook is good. Most people recover quickly and completely. If you had complicated appendicitis, your recovery might take longer. You might need repeat treatments for infection that spread beyond your appendix. Appendicitis that’s treated with antibiotics alone has a return rate of 40%. Appendicitis that goes untreated has a mortality rate greater than 50%.